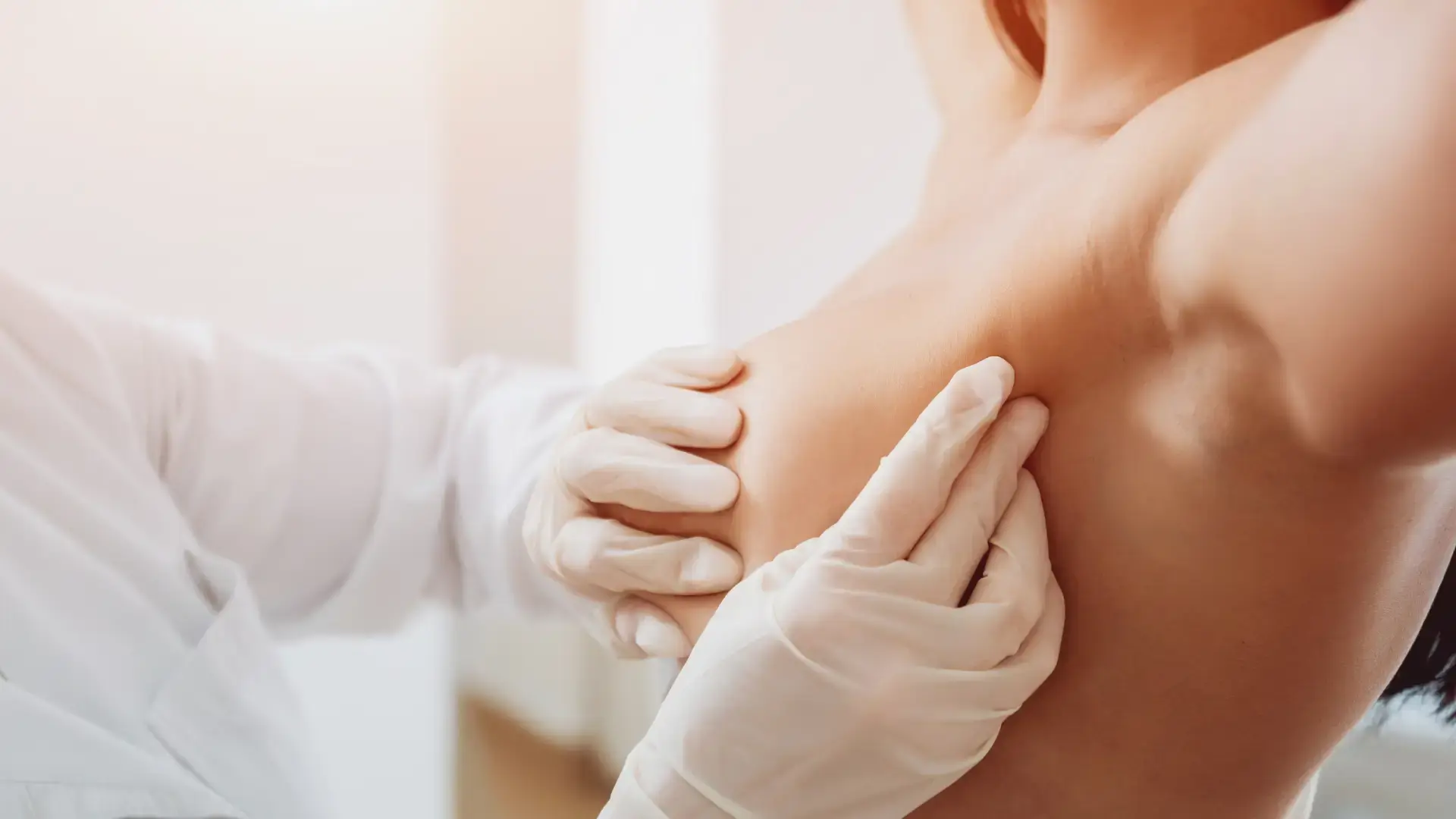
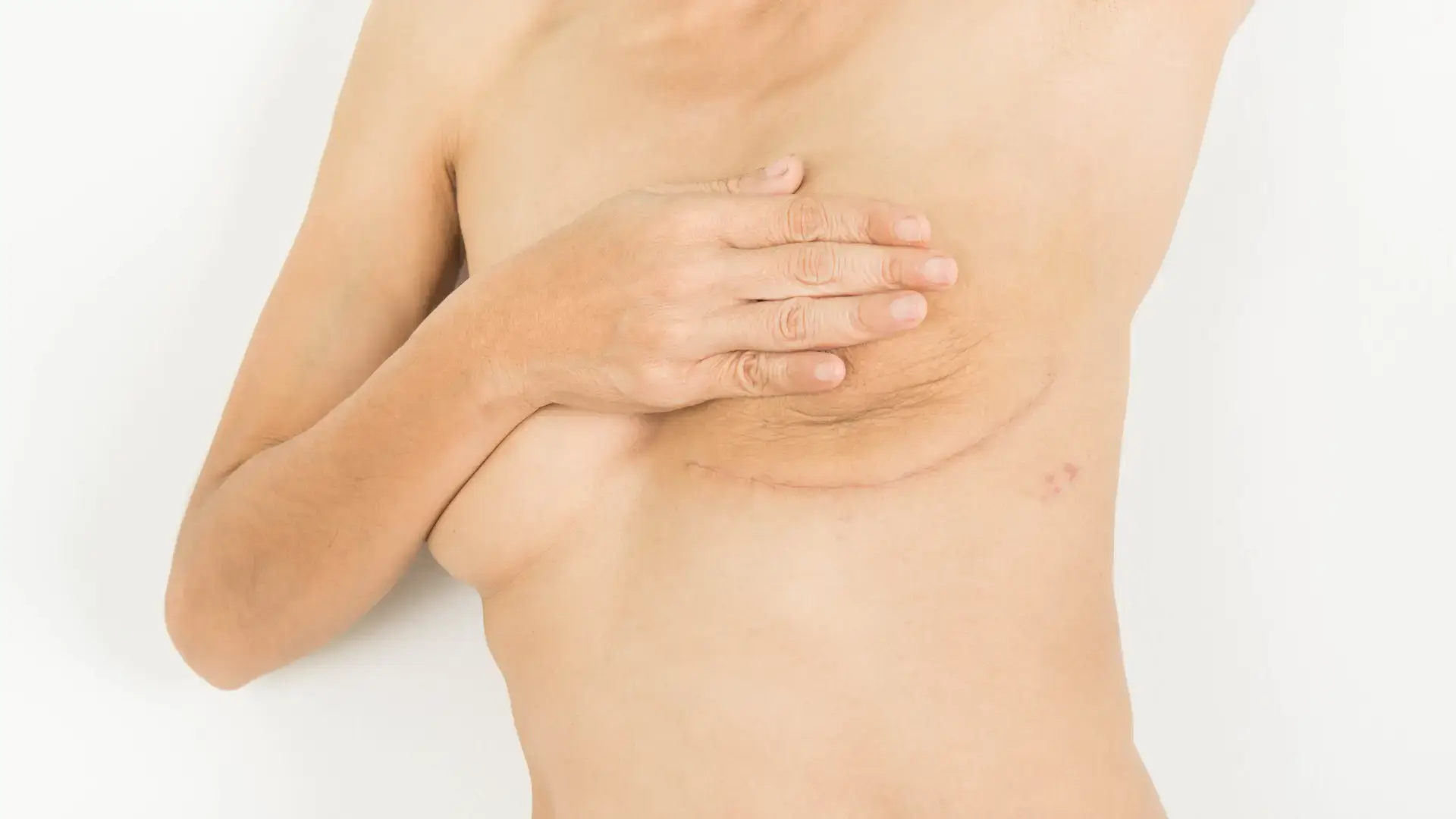
If you’ve noticed a small bulge during a bowel movement, light bleeding, or a feeling of pressure th...
The Premier Surgical Network Blog offers the latest updates, expert insights, and in-depth articles on the evolving field of surgery. From cutting-edge technologies to new treatment approaches, our blog provides valuable information for healthcare professionals and patients alike, keeping you informed on the advancements shaping the future of surgical care.


.webp)

.png)
.webp)